Department Overview
Department of Paediatrics and Neonatology is situated on the first floor of Symbiosis Medical College for Women and Hospital, in the picturesque Lavale hill base campus, Pune. The department provides comprehensive health care and protocol-based treatment and cure to every child attending the OPD, Emergency room or admitted in paediatric wards, NICU or PICU. It nurtures and supports every child to live a healthy life and develop to fullest potential.

Vision
To provide comprehensive health care to children and neonates and to impart quality paediatrics education to medical graduates with thrust on empathy and compassion.

Mission
- Imparting competency based dynamic education to medical graduates for essential new-born, child and adolescent health care that puts the needs of learners first.
- Improving child health care through clinical research and innovative technologies
- Providing community-based adolescent and child health care by effective extension services and counselling.
- Promoting quality and patient safety.
- Developing leaders and professionals in child health and research.
HOD Profile

Dr Anjali Milind Kher
MBBS; MD(Paediatrics); MPhil (HPE)
Experience
Dr Anjali Kher has been working as a paediatrician and neonatologist for 33 years, has a teaching experience of 19 years for medical undergraduates and 6 years of experience as postgraduate teacher and guide in Paediatrics. She has worked for neonatal and child health right from grass root level to tertiary care. She has a passion for teaching and is interested in research. She is a strong believer in lifelong learning and tries to inculcate the same attitude in her students.
Dr Anjali Kher has given many radio talks, phone in programs on AIR and worked a lot in HIV awareness, malnutrition and breastfeeding promotion and support. She has worked in various government civil hospitals, government medical college Nagpur, many non-governmental organizations and private medical colleges before joining SMCW, Pune.
Achievements
- Dr Anjali Kher has conducted undergraduate and postgraduate practical examinations in Paediatrics in government and private medical college as an external examiner, internal examiner and convener. She has chaired sessions in state and national conferences. She has presented poster and paper in conferences.
Paper Publications
Dr Anjali Kher has 23 paper publications in many international and national journals and many of them as first or corresponding author.
Outreach activities
Dr Anjali Kher has delivered many interactive lectures as guest speaker for Anganwadi workers, Supervisors, ANM sisters and MO during their training programs. She has conducted many healthy baby competitions and attended many health camps as paediatrician in peripheral PHC, CHC and Anganwadi.
Paediatric Department

The Department of Paediatrics includes a Department Office, Paediatric OPD, Paediatric Ward, NICU, PICU. It was established in August 2019 with a team of Doctor Counsellor and support staff.
The Out Patient Department (OPD)


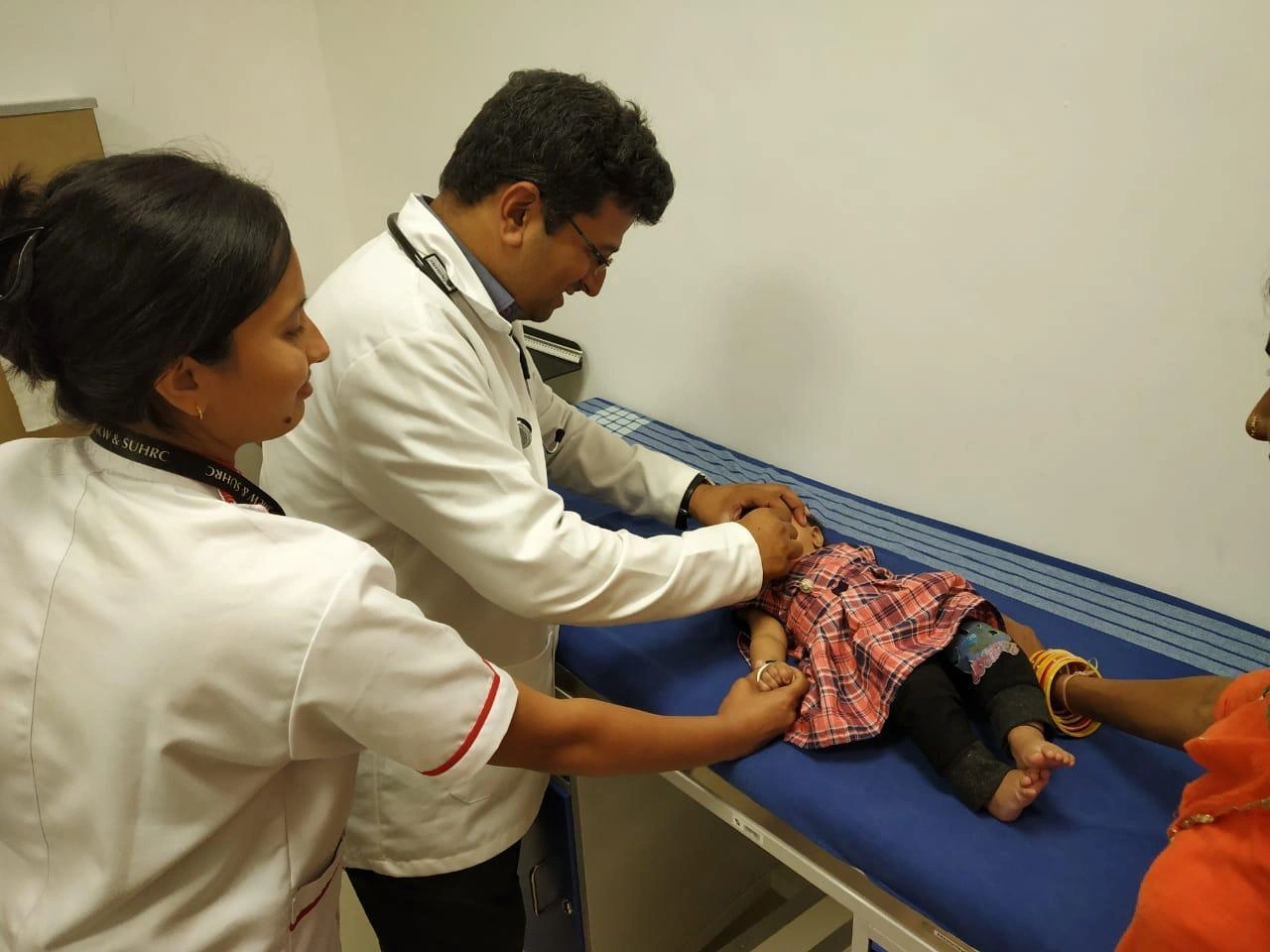

(OPD) is child friendly and well equipped with examination rooms, immunization room, well baby clinic, child guidance room, treatment room, waiting area and play station for patients, demonstration room and feeding room.
In Patient Department (Paediatric Ward)
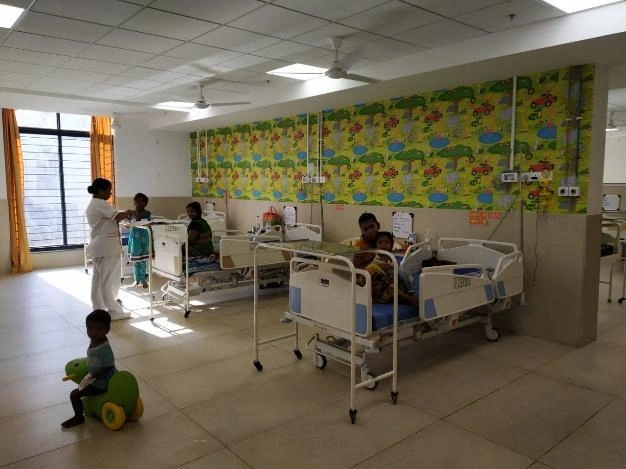

IPD comprises of three wards with 25 beds in each ward and nursing station overviewing the beds and 9 beds are available with facilities of central oxygen and suction. It consists Isolation unit, teaching area demonstration room, Treatment room, Duty doctor room, Side laboratory, Dirty utility room.
Neonatal Intensive Care Unit
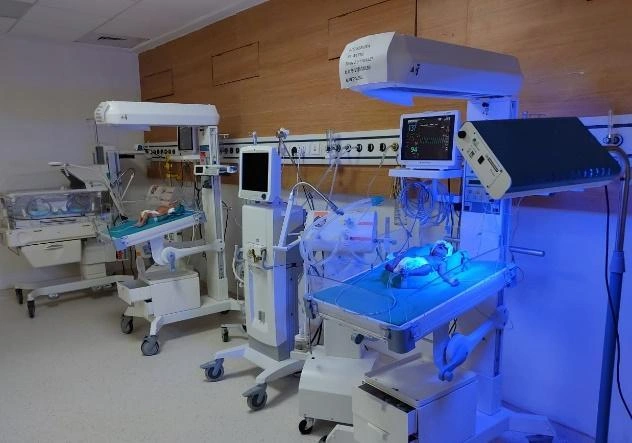
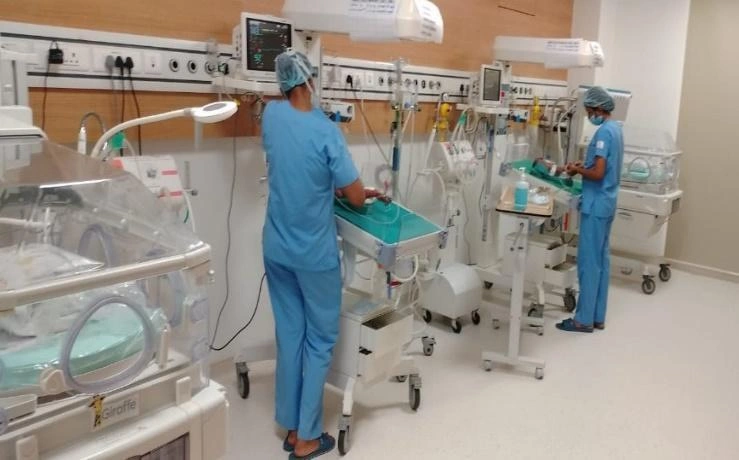



Two NICU level-III consisting of 5 beds in each tertiary (Level III) NICU
Two separate cabins- high dependency and low dependency area, Isolation area for septic babies, feeding room with KMC, Central nursing station, duty Doctors room.
One Step Down NICU (Level II) consisting of 5 beds with warmers, incubator central oxygen, phototherapy units, feeding room with KMC, Central nursing station, duty Doctors room.
Paediatric Intensive Care Unit

PICU consist of 5 beds with critical care facilities inclusive of Ventilators and caters to all critically ill paediatric patients and consists, Central nursing station, duty Doctors room.
Meet Our Faculty
Dr. Anjali Kher
MBBS, MD (Paediatrics), MPhil (HPE)
Professor & HOD
anjali.kher@smcw.siu.edu.in
Col (Dr) A.R. Rajan (Retd)
MBBS, MD (Paediatrics)
Professor
allampalam.rajan@smcw.siu.edu.in
Dr. Shweta Dhasal
MD (Paediatrics), DCH, MBBS
Assistant Professor
shweta.dhasal@smcw.siu.edu.in
Dr. Nitin Lingayat
MBBS,DCH,DNB,FIAP Neonatalogy (Paediatrics)
Associate Professor
shridhar.jadhav@smcw.siu.edu.in
Dr. Amit Rathod
MBBS, MD (Paediatrics)
Associate Professor
amit.rathod@smcw.siu.edu.in
Dr. Shridhar Jadhav
MBBS, MD, DFPCCN (Paediatrics)
Associate Professor
shridhar.jadhav@smcw.siu.edu.in
Maj. (Dr.) Ved Pratap Tiwari, Retd
MD (Paediatrics), MBBS
Associate Professor
ved.tiwari@smcw.siu.edu.in
Research Publications
Services
The department along with PSM department has regular outreach health facility at Rural and Urban health centres at Male and Pashan respectively
Department carries out regular immunization program and pulse polio immunisation as well.
Department provides various developmental screening tests, intelligence tests, autism screening test, psychological and family counselling.
Regular breastfeeding promotion and nutrition counselling services.
Services provided in OPD
Diagnostic and therapeutic services for out-patients (new-born to adolescent)
| Name of the Clinic | Weekday/s | Timings | Number of cases (average) | Name of Clinic In-charge |
|---|---|---|---|---|
| Paediatric Cardiology | Wednesday | 9am To 1pm. | 04 |
Dr. A.R. Rajan
Dr Abhishek Saklecha
|
| Paediatric Nephrology | Thursday | 9am To 1pm. | 03 |
Dr Anjali Kher
Dr Girish Kumthekar
|
| Paediatric Endocrine | Monday | 9am To 1pm. | 03 |
Dr. Amit Rathod
Dr. Sarang Barbind
|
| Paediatric Neurology | Friday | 9am To 1pm. | 05 |
Dr Deepak Joshi
Dr. Savali Sutane
|
| High risk Follow up clinic | Friday | 9am To 1pm. | 05 |
Dr. Shridhar Jadhav
|
| Immunization | Monday, Tuesday, Thursday, Friday | 9am To 1pm. | 29 |
Dr. Anjali Kher
Dr. A.R. Rajan
Dr. Deepak Joshi
|
| Paediatric Asthma | Tuesday | 9am To 1pm. | 08 |
Dr. Deepak Joshi
Dr. Minakshi. B
|
| Child Rehabilitation | Tuesday, Thursday | 9am To 1pm. | 15 |
Dr. Pooja Agrawal
|
| Nutritional Rehabilitation Clinic (NRC) | Tuesday | 9am to 1pm | 10 |
Dr. Amit Rathod
Dr. Priscilla Marian
|
| Child guidance clinic | Daily | 9am to 1pm | 04 |
Dr. Anjali Kher
Miss. Geeta Nikam
|
| Counselling services | Daily | 9am to 1pm | 10 |
Miss. Priya Pathak
|
| Well baby | Monday & Wednesday | 9am To 1pm. | 12 |
Dr. Nitin Lingayat
|
- Treatment room for handling any emergency, Nebulization facility.
- Speciality Clinics available in OPD - Paediatric Neurology, Paediatric Cardiology, Paediatric Nephrology, Paediatric Endocrinology, Paediatric Asthma clinics.
Services provided in Paediatric wards:
- Diagnosing and treating children with common childhood illnesses- Diarrhoea, respiratory infections, nutritional disorders and malnutrition.
- Assessing and providing intervention for abnormalities in growth and development
- Diagnosing and treating renal, endocrine disorders, cardiac illnesses, neurological diseases, childhood asthma, adolescent health issues
- Transfusion of Blood and Blood products.
- Spirometry (With Department of Respiratory Medicine) and PEFR for asthma
Services in the NICU :
- Care of all critical patients admitted in NICU including very low weight and extremely low birth weight babies.
- Treatment of common neonatal diseases like Sepsis, Asphyxia, Convulsions, Hypoglycaemia etc.
- Fluid and electrolyte management and other neonatal care.
- Advanced neonatal resuscitation.
- Advanced mechanical ventilation.
- Surfactant administration.
- Phototherapy and Exchange Transfusion for neonatal Hyperbilirubinemia
- Family centred New-born care for Preterm and High Risk New-borns
- Developmentally Supportive care
- KMC practice
- Supporting and promoting Exclusive Breast Feeding Practices
- Bedside functional Echocardiography.
- Bedside Neurosonography
- Transfusion of Blood and Blood products
Services in PICU :
- Paediatric critical patients are admitted in PICU.
- Mechanical Ventilation.
- HFNC oxygen therapy.
- Bedside functional Echocardiography.
- Bedside Neurosonography, Sonography and X rays.
- Transfusion of Blood and Blood products.
- Treatment of critical paediatric patients with Meningitis, Encephalitis, Status epilepticus, Status Asthmaticus, Acute Renal Failure, Shock, Severe Pneumonia, etc.
Key Focus Areas
The identified Thrust areas for research focus
1. Neonatology-
ENAP- Every Newborn Action Plan - by UNICEF & WHO- to to end preventable newborn
Deaths and stillbirths by 2030- Focus Areas:
1. Neonatology-
ENAP- Every Newborn Action Plan - by UNICEF & WHO- to to end preventable newborn
- Data & Measurement: Improving the quality and availability of data on newborn care, including equity and quality gap assessments.
- Quality Care: Promoting quality improvement initiatives for maternal and newborn health (MNH) to ensure proper care at and around birth, reduce prematurity & infection
- Essential Commodities: Ensuring the availability of necessary medical supplies for newborn care.
- Equity: Working to reduce disparities in care and close health equity gaps.
2. Nutrition-
- Neonatal feeding & Breast Feeding
- Preschool, school & Adolescent Nutrition- Stunting & wasting
- Child Obesity
- Community nutrition education and awareness- Anganwadi/school/hospital
3. Acute Respiratory Infection-
- LRTI, Bronchiolitis
4. Vaccination-
- Vaccine coverage and reminder apps (E platform)
- PICU admissions and vaccination received by these children (HIB/Pneumococcal/ Rota viral)
The department's three key focus areas are clinical care, education and research.
- Comprehensive lactation Management
- Child and adolescent nutrition
- Preventive health care in paediatrics focused on the concept of developmental origin of health and disease (DOHaD) and thousand days
- To impart competency based medical education to medical students and allied health sciences students
- Clinical research and innovations in child health care
Upcoming Departmental FDP, Conference
Faculty Development Programme (FDP) Proposal:
- Paediatric Advanced Life Support (PALS)
- Concept Note
- Title of the FDP Paediatric Advanced Life
- Support- SMCW-SUHRC -Proposed by Department of Paediatrics,
- Target Audience Faculty (Assistant Professor and above) and Senior Residents from Paediatrics, Phase 111 Part 11 MBBS students
- Proposed Duration July 2026; 1 Day - Total 8 hours of Instruction
- Mode Lectures; Manikin
- Expected Batch Size 30
- Venue Dept. of Paediatrics and Moringa Auditorium
Expected Learning Outcome:
Participants are expected to be able to:
- Master PALS Content: Deepen knowledge of the systematic approach to paediatric assessment, respiratory emergencies, shock management, and cardiac arrest algorithms.
- Demonstrate Instructional Proficiency: Effectively deliver PALS core concepts, conduct engaging lectures, facilitate skills practice sessions, and manage simulation scenarios
- Evaluate Learner Performance: Apply standardized evaluation methods to assess student competency in BLS, PALS skills, and scenario management.
- Promote Effective Team Dynamics: Teach and model high performance team behaviours’, clear communication, and leadership roles during resuscitation.
- Adhere to Program Standards: Understand and comply with the administrative and quality control requirements for running official PALS courses (e.g., American Heart Association or equivalent organization guidelines).
Programs
Elective 1 & 2
| Name of the block | Block 2 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Name of the elective | "Prematurity in Neonates" | ||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Name of the hospital | Symbiosis Medical College for Women | ||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Name of the internal preceptor |
Dr Amit Rathod Dr Nitin Lingayat Dr Anjali Kher |
||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Name of the external preceptor if applicable | NA | ||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Specific learning objective |
At the end of this Module student should be able to:
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Number of students that can be accommodated in this elective | 5 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Pre-requisites for this elective |
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Module Structure |
Week 1: Introduction & Basics
Week 2: Systems & Complications
Week 3: Long-Term Issues & Multidisciplinary Care
Week 4: Integration & Assessment
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Teaching Methods |
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Assessment Methods (Formative & Summative) |
Formative (throughout):
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Log book entry required | Satisfactory completion of elective by a preceptor with a satisfactory grade | ||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Resources Needed |
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Other Comments |
| Name of the block | Block 2 |
| Name of the elective | “Development in Children” |
| Name of the hospital | Symbiosis Medical College for women |
| Name of the internal preceptor |
Dr A R Rajan Dr Anjali Kher Dr Deepak Joshi Mrs Geeta Nikam |
| Name of the external preceptor if applicable | NA |
| Specific learning objective |
At the end of this Module student should be able to:
|
| Number of students that can be accommodated in this elective | 5 |
| Pre-requisites for this elective | 1. Phase III Students |
| Module Structure |
Week 1: Fundamentals of Growth & Development
Week 2: Developmental Screening & Early Detection
Week 3: Developmental Disorders & Interventions
Week 4: Early Stimulation, Parent Counseling & Community Perspective
|
| Teaching Methods |
|
| Assessment Methods |
Formative:
|
| Log book entry required | Satisfactory completion of elective by a preceptor with a satisfactory grade |
| Resources Needed |
|
| Other Comments |
Value Added Course
1.Soft Skills in Paediatrics
Ideal Audience:
MBBS 5th–9th semester (before or during Paediatric postings)
Total Duration: 36 Hours
Module-Wise Breakdown
- Module 1: Foundations of Paediatric Communication – 3 hours
- Module 2: Paediatric History Taking as a Conversation – 4 hours
- Module 3: Talking to Parents – The Toughest Part – 4 hours
- Module 4: Counselling for Common Paediatric Conditions – 4 hours
- Module 5: Breaking Bad News in Paediatrics – 4 hours
- Module 6: Soft Skills in Procedures & Emergencies – 3 hours
- Module 7: Working in Teams, Handover & Professionalism – 3 hours
- Module 8: Ethics, Child Rights, Confidentiality & Digital Conduct – 3 hours
Skills Labs – 6 hours
| Lab | Duration | Focus |
| Skills Lab 1 | (2 hours) | Role-plays with constructive peer + faculty feedback |
| Skills Lab 2 | (2 hours) | Simulated parent–doctor–child interactions (record + review) |
Clinical Shadowing & Reflective Learning: 4 hours
Assessment – 2 hours
OSCE (5 stations):
- Breaking bad news
- Immunisation counselling
- Procedure communication
- Angry parents scenario
- Handover using SBAR
- Mini Viva
- Portfolio Submission (reflection + micro-counselling script)
Certificate: Awarded only after passing OSCE + completing portfolio.
2.Lactation Counselling & Breastfeeding Support
Total Duration: 36 hours (Blended: Theory + Skills + Clinical + Assessments)
Course Purpose
Equip MBBS students with practical, hands-on skills in breastfeeding support so they can assess feeding issues, guide mothers, and provide first-line counselling during postings or internships.
Learning Outcomes
By the end of 36 hours, students will be able to:
- Explain breastfeeding physiology and benefits
- Demonstrate proper latch, positioning and attachment techniques
- Assess a breastfeeding session using structured tools
- Manage common breastfeeding challenges and myths
- Support lactating mothers in hospitals, NICU, community, and via tele-counselling
- Communicate sensitively and effectively with parents
| Module | Topic | Hours | Method |
| 1 | Why Breastfeeding Matters | 2 | Interactive lecture + videos |
| 2 | Anatomy & Physiology of Lactation | 3 | Lecture + short quiz |
| 3 | Early Initiation (ENBC) & First 48 Hours | 3 | Demo + role play |
| 4 | Effective Breastfeeding Techniques | 5 | Hands-on with models + peer practice |
| 5 | Breastfeeding Assessment Skills | 3 | OSCE style skill station |
| 6 | Common Problems & Solutions | 5 | Case-based learning + skill practice |
| 7 | Preterm, Sick & NICU Babies | 3 | Neonatology session + videos |
| 8 | Communication & Counselling Skills | 4 | Role play + feedback |
| 9 | Medications, Working Mothers, Milk Expression, Storage | 3 | Practical demo + infographics |
| 10 | Breastfeeding in Public Health Programs | 2 | RBSK, IYCF, BFHI, MAA |
| 11 | Evaluation & Certification | 3 | OSCE + viva + reflective assignment |
Teaching & Learning Methods
- Mini-lectures (max 20–30 min each)
- Demonstrations with breastfeeding manikins
- Supervised practice with mothers (wards/NICU)
- Case-based discussions
- Role play of counselling scenarios
- Audiovisual training clips
- OSCE skill stations
Assessment
- Formative (10 marks): Participation + worksheets
- Skill OSCE (40 marks): Latch, positioning, counselling
- Theory MCQ/short answer (40 marks)
- Reflective journal (10 marks): 3 real counselling encounters
Certification Criteria
- Minimum 80% attendance
- Pass in theory + OSCE


